Which symptoms and signs do Lyme disease cause and how does the disease progress? How does it feel to have Lyme?
Lyme disease is transmitted when a tick is feeding. When an infected tick has attached itself there is a risk that the disease is transmitted.
NOTE: Do not miss our 10-minute online test which calculates your Lyme disease risk level based on symptoms and their occurrence.
Erythema migrans (redness of skin around tick bite)
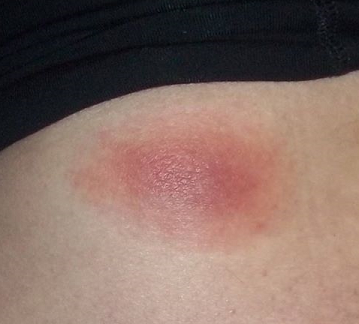
Three to thirty days after the tick bite around 50% of all infected people in northern Europe develop a redness around the tick bite (Thl.fi, 2016). The shape may be oval or more irregular. This poster provides a good overview of this stage of the disease with some example pictures. Note that the central clearing is rare – it is more common just to have a filled red shape. The redness continues to grow in the upcoming weeks and may become larger than 30 cm in diameter. Additional redness may appear on other areas of the body (Netdoctor.co.uk, 2012), but this means that the disease has entered the “Early disseminated disease” phase which is described in the next chapter.
If you get such a redness, take a good close-up picture and another picture which shows that it’s you on the picture. The reason for this is that the redness might disappear before you have the chance to see a doctor. Go see a doctor as quickly as possible, every day is important in reducing the risk for long-term complications because the bacteria replicates quickly and will try to hide deeper in the body.
If treatment is started in this early phase the redness usually starts to shrink again after around one day and disappears after one to two weeks.
Blood samples does not work in this early phase because they rely on the body to first produce antibodies. Creation of such antibodies may take 4 to 6 weeks. Treatment in this phase of the disease shall therefore be given without waiting for test results.
Early disseminated Lyme disease
A few weeks after the tick, as the bacteria is spreading in the body, some get flue-like symptoms (Healthline, 2018). It may feel like a protracted cold or flue that does not really get started. You may have a feeling that something is not right in the body and very often fatigue occurs. Usual symptoms are:
- Flue-like symptoms
- Low-grade fever
- Enlarged lymph nodes, e.g. on the neck
- Tiredness
- Pain in the body
- Headache
Lyme neuroborreliosis
A few days to months after the tick bite the bacteria may succeed in passing the blood-brain barrier. The disease then starts to give more neurological manifestations. This phase of the disease is called “Lyme neuroborreliosis”.
Lyme neuroborreliosis often starts with back pain, e.g. in between the shoulder blades or in the neck (Netdoctor.co.uk, 2012). This pain will often worsen at night.
Other common symptoms include:
- Headache – it may move around the head during the day or from day to day.
- Nerve symptoms – e.g. pain, tingling, pins/needles, burning feelings, numbness or paralysis in different parts of the body. It is common that the facial nerves are affected and this may in some cases result in that one or both sides of the face starts to hang a little (Bell’s palsy). It is also very common that feet and/or hands are affected by these sensations.
- Problems to concentrate and remember things
- Sleeping problems
- Depression, mood swings and/or anxiety
Pain killers rarely works well for the pain and/or headaches that Lyme disease cause.
Diagnosis of Lyme neuroborreliosis
If Lyme neuroborreliosis is suspected, the doctor may decide to perform a lumbar puncture test. This is a test where the doctors put a needle in the back in order to extract some spinal fluid.
Doctors and researchers in the German medical Lyme disease association “Die Deutsche Borreliose-Gesellschaft” advice against performing this test if a long time has passed since the suspected infection as there then is a significant risk that the the test misses the Lyme disease. The lumbar puncture test relies on antibodies to be present in the spinal fluid. The German Lyme disease association notes that such antibodies may be missing both in early and late stages of the disease. In general, they note that the lumbar puncture test has a low chance of detecting Lyme disease (section 2.5.3 in the document Deutsche Borreliose-Gesellschaft, 2010).
There are also risks involved with performing a lumbar puncture. The needle may damage a nerve which can give lengthy complications. There is also a risk that a blood vessel is damaged when the needle enters and that blood therefore end up in the spinal fluid.
Other complications of Lyme disease
Lyme disease can essentially give three other main complications:
- Lymphocytoma – a red or blue lump/swelling, often located on the ear lobe or the outer side of the ear. It may also occur on other parts of the body.
- Acrodermatitis – blue/red skin lesions, often located on the knuckles of the hands or feet. Bacteria is eating it’s way through the skin and the skin becomes more thin – it may feel like kitchen towels when touched. Sometimes the upper side of a whole hand or feet is affected. Acrodermatitis may also affect other parts the body and has a slow progression (Dermnetnz, 2015). It is common to also have peripheral neuropathy at the same time, which may feel like burning sensations at the very same location as the skin lesions.
- Lyme arthritis – swelling in one or several larger joints (e.g. a knee joint), either of acute or relapsing nature. Inflammation often cause pain and/or swelling. Often only one joint is affected and it is rare that more than three joints are inflamed. With treatment the swelling disappears after one to four weeks but may return again after months to years (Netdoctor.co.uk, 2012).